How CBT works for Excoriation Disorder?
One of the reasons why it’s so hard to find appropriate treatment for skin picking is that it was recognized by the American Psychiatric Association as a mental health problem only in 2013. Even after 2013, it may be the case that your therapist or your psychiatrist don’t know how to approach this “novel”, newly recognized problem. SkinPick has developed an online therapy program mainly to fill in this gap in treatment availability, by providing care that is not only affordable and available everywhere in the world, but care that is evidence-based, grounded in research and science, yet flexible enough to encompass the wide variety of our lived experience as human beings.
What makes this program so flexible and affordable is that it’s a form of internet-based CBT. Studies are now emerging with increasing regularity that show the effectiveness of administering CBT in this way, for a wide variety of conditions. A comprehensive metanalysis showed that in person and online CBT have equivalent results
What is CBT for Excoriation Disorder?
CBT is the most common mode of treating body-focused repetitive behaviors. In addition to being the most common approach, it’s also the one that has been tested the most, and because we wanted to provide evidence-based support, building our program with CBT tools was the logical choice.
After half a century of development, it’s best to think about CBT not as just a form of therapy, but an umbrella for different therapeutic modalities that share some common ideas and principles. What separates CBT from other forms of “talk therapies” is that the focus is on how our thoughts, feelings and actions influence each other as the primary focus. CBT is a proactive and practical approach to therapy that looks to incorporate behavioral change and create practical difference in one’s life at the expense of understanding the psychodynamic nature of the problem.
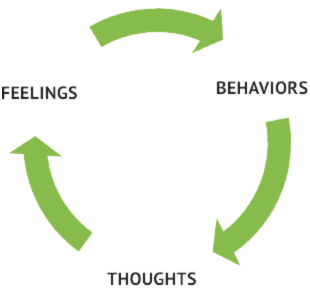
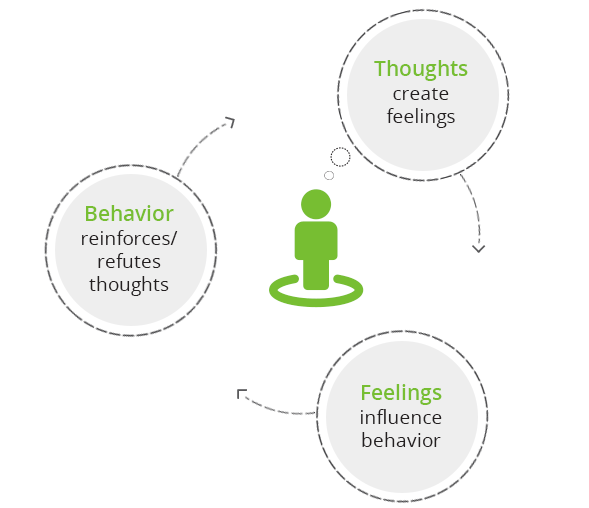
Because of the many different approaches to CBT, it’s difficult to present a generalized model. We can say that in CBT, therapists strive to make their clients aware of how their thoughts cause certain feelings which, in turn, lead to dysfunctional behaviors. These behaviors create more negative thoughts and feed into the cycle further. In our day-to-day life, we are usually unaware of this cycle. Once we make ourselves aware of it, we are able to apply different strategies and interfere in different parts of this cycle, either by relating to our thoughts or feelings differently, or by consciously altering our behaviors.
Habit Reversal Training (HRT)
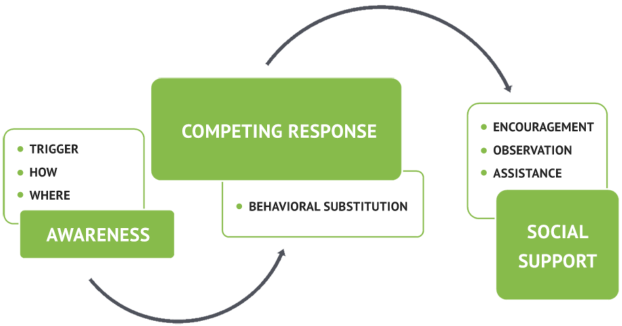
HRT is a behavioral intervention that helps you replace picking with a healthier kind of behavior that achieves a similar effect. HRT has several distinct stages that have to unfold in a specific order for the treatment to work well. It starts with a stage that we call awareness training in which you monitor your skin picking, as well as associated thoughts and emotions, in order to be aware of the behavior, identify triggers and understand how thoughts and emotions lead to picking.
Acceptance and Commitment Therapy
Once you complete HRT, you slowly move on to another form of treatment based on acceptance and commitment therapy – ACT. In the first part, HRT helped you take control of picking and gave you the option to choose healthier behavior when the urge to pick arises. ACT will help you deal with the urge itself.
ACT is a part of what is known as the third wave of CBT. That means that in addition to standard CBT features described in the beginning of the page, ACT implements other tools as well. Some of the tools that you will learn how to use include acceptance, mindfulness, cognitive defusion, as well as behavioral commitment that stems from your values.
In this type of CBT, we look at picking as a form of experiential avoidance, a mechanism employed to avoid intense and difficult emotional experience. Succinctly put, hair pulling comes about as a way to cope with but not fully process those difficult experiences. From the ACT point of view treatment consists in learning a different approach to our own experience, one of acceptance, mindfulness and detachment that allows us to be with our feelings but not get overwhelmed by them.
Does CBT work for excoriation disorder?
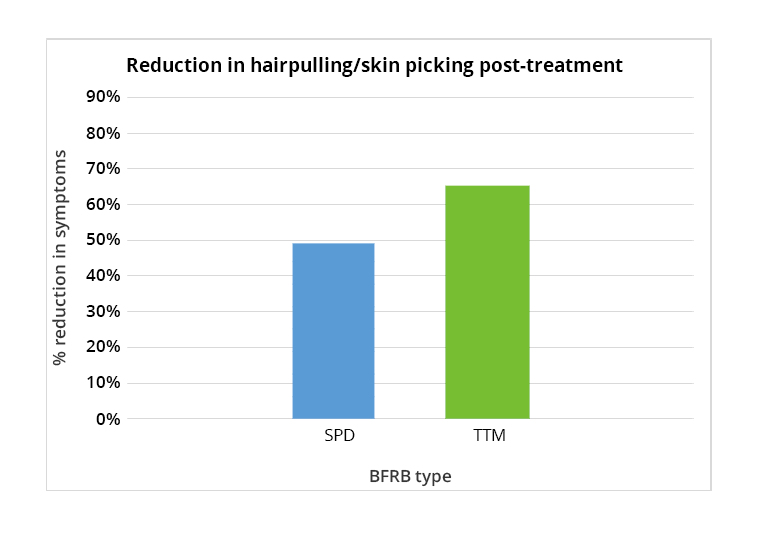
CBT is recognised among health professionals as the most effective method of treatment for BFRBs such as excoriation disorder. A recent survey of treatment options listed both HRT and ACT as evidence-based, successful interventions. Furthermore, a study conducted by researchers at the University of Heidelberg showed that specifically internet-based CBT can be a helpful, effective intervention for people struggling with skin picking.
One study looking at the effectiveness of ACT and HRT found that there was a significant reduction in skin picking frequency (49.5%) in the participants who received ACT/HRT compared to those who were in the control group. Another study examined the effects of brief cognitive-behavioral therapy for pathological skin picking based on measures of severity of skin picking, psycho-social impact of skin picking, and it included a two months follow-up assessment. The results showed a significantly large reduction on all measured variables, with treatment effects maintained at 2 months follow-up.