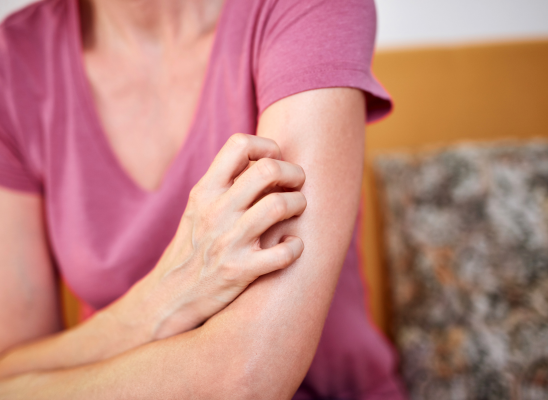
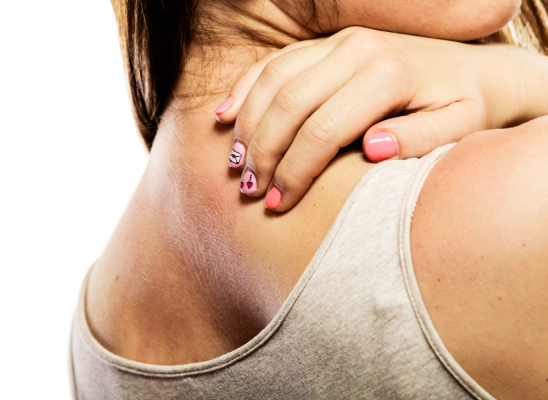
How A Little TLC Can Help Your Skin Picking
Online test
Find out the severity of your symptoms with this free online test
Braving BFRBs: Expert Insights on Skin Picking & Hair Pulling
Braving BFRBs: Expert Insights on Skin Picking & Hair Pulling – a free webinar series brought to you by SkinPick!
Join Meryl Da Costa-Rohland, Counsellor and Community Manager at SkinPick, as she sits down with clinical psychologists Dr. Sofia Wenzler and Vedrana Mirkovic to explore the emotional and psychological challenges of skin picking and hair pulling.
Through honest conversations and expert guidance, you’ll gain practical tools, new insights, and a sense of connection. Whether you're on your own recovery journey or supporting someone else, this series offers knowledge, compassion, and hope.

Online Test for Skin Picking
How Severe is Your Picking Disorder? Find Out With This Free Online Test
Take the testStart your journey with SkinPick
Take control of your life and find freedom from skin picking through professional therapy and evidence-based behavioral techniques.
Start Now