Concerned About Picking Your Skin?
Online test
Find out the severity of your symptoms with this free online test
It is not uncommon for people to subconsciously rub, touch, or scratch at their skin, just as it is a common practice for many people to pick at skin imperfections such as acne or blackheads. However, for some, this practice becomes so consuming that it is classified as a skin picking disorder known as excoriation disorder or dermatillomania. Picking your skin becomes problematic when the picking is repetitive and it becomes difficult for the person to voluntarily stop engaging in the behaviour, and impacts negatively on daily functioning. This poorly understood problem often goes undiagnosed and therefore untreated.
Online Test for Skin Picking
How Severe is Your Picking Disorder? Find Out With This Free Online Test
Take the testHow will I know if I have skin picking disorder?
Regular picking at pimples or other perceived skin imperfections does not necessarily mean you have skin picking disorder. There are very specific criteria that define the disorder, distinguishing it from other conditions that may present with similar behaviours. For example people with Body Dysmorphic Disorder (BDD), who have obsessive thoughts about perceived flaws in their appearance (either real or imagined) may also pick at their skin to remove these imperfections. There are also those who have suicide ideation or intentionally self-harm as a form of emotional release. While these behaviours may appear to have similarities with skin picking disorder, it is the combination of criteria and patterns of behaviour that distinguishes one from the other. If you are concerned that you may have a skin picking disorder, there is a possibility that the behaviour has escalated to an extent that warrants concern. In this case it is advisable to seek medical advice. Diagnosis of skin picking as a disorder is based on the criteria outlined in the Diagnostic and Statistical Manual 5 (DSM 5) as follows:
- Recurrent skin picking resulting in skin lesions
- Repeated attempts to decrease or stop skin picking
- The skin picking causes clinically significant distress or impairment in social, occupation, or other important areas of functioning
- The skin picking is not attributable to the psychological effects of a substance (e.g., cocaine) or another medical condition (e.g., scabies)
- The skin picking is not better explained by symptoms of another mental disorder (e.g., delusions or tactile hallucinations in a psychotic disorder, attempts to improve a perceived defect or flaw in appearance in body-dysmorphic disorder, stereotypes in stereotypic movement disorder, or intention to harm oneself in non-suicidal self-injury)

There is no definitive pattern of picking as the where, when, and how people pick at skin varies. While the most common area to pick skin is the face, picking can occur anywhere on the body where there is skin. Some other common areas include the back, shoulders, arms, legs and scalp. Some people pick only with their fingers or dig into their skin with their finger nails, while others use their teeth, or tools such as tweezers, pins or any other sharp objects they have access to.
If you suspect you may have skin picking disorder, you should visit a health professional and express these concerns. However, awareness about skin picking disorder is still limited, even among the health fraternity. Having some knowledge about the condition and these criteria when you visit your health practitioner is therefore recommended.
Why can’t I stop picking my skin?
As seen from the DSM5, one of the criteria for diagnosis is that repeated attempts to stop picking are evident. Even if you know you should not pick or want to stop picking at your skin, doing so is incredibly challenging. This inability to stop picking is often a source of intense shame, guilt and a sense of failure. Picking is often precipitated by an urge, which the individual is unable to resist. However, sometimes picking happens automatically without the individual being overtly aware of their action until they have already picked. The underlying reasons or stimuli for picking also vary from person to person. Automatic picking most commonly occurs when the person is idle, bored, or engaged in passive activities such as watching television. Focussed picking is often precipitated by negative thoughts or emotions, or an inability to cope with stress, anxiety or tension. Most people challenged by skin picking disorder describe a sense of satisfying relief or release of tension immediately after picking, but this is quickly followed by feelings of intense shame.
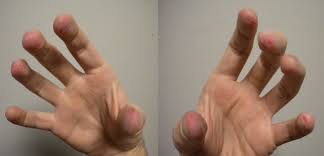
Will I cause permanent damage?
While it may be possible to repetitively pick your skin without causing permanent damage, the risk of developing infection, tissue damage or scarring at the site of picking is ever present. You can tell that your skin has become infected if it is red, warm and tender. It is best to seek medical assistance if the infected area does not heal quickly or appears to be spreading. The deeper into the layers of the skin you pick, the more likely it is that scarring will occur. This is because picking deep below the top layers of the skin to the dermis and beyond, removes the pigment that gives the skin its color. It may take months for the skin to return to its normal color, or it may remain permanently discoloured.
I don’t know anyone else who picks their skin
According to the OCD Foundation, as many as 1 in 20 people are affected by skin picking disorder and it occurs in both men and women. In fact, studies indicate that 2% of all dermatology patients and 4% of college students pick their skin to the point where it causes noticeable tissue damage and marked distress or impairment in daily functioning. It is important to remember that you are not alone with this problem, even though awareness of this condition is sorely lacking.
Can I get help?
Although there is help available for skin picking disorder, awareness of the condition is lacking and therefore few medical and mental health professionals are adequately trained to treat the behavior successfully. Organizations such as the Trichotillomania Learning Center (TLC) keeps a database of treatment professionals who are knowledgeable about this disorder and can help you in your search for a local treatment provider. If there is not a professional accessible in your area, it is advisable to seek out psychologists and therapists who specifically specialize in cognitive-behavioural therapy and habit reversal training. Self-education and self-help therapy programs are also available online at websites such as skinpick.com. This option is especially helpful if you have limited resources to access face-to-face individualized therapy. The more people recognize the signs and symptoms of the condition, the more people will be formerly diagnosed, which will have a positive ripple effect on awareness and development of greater treatment options over time.
Online test
Find out the severity of your symptoms with this free online test
Start your journey with SkinPick
Take control of your life and find freedom from skin picking through professional therapy and evidence-based behavioral techniques.
Start Now



