Online test
Find out the severity of your symptoms with this free online test
People who have limited knowledge about skin picking often do not consider it as a serious problem. Awareness about excoriation disorder has only recently taken an upsurge with relatively few people knowing that such a condition even existed just a few years ago. Those with it usually feel embarrassed or ashamed to discuss it as many people misunderstand it. People that suffer from dermatillomania exhibit symptoms that include repetitive touching, rubbing, scratching, picking at, and digging into their skin. Some people do this to remove irregularities or perceived imperfections while others do it obsessively for other reasons such as relieving stress or just being bored. The behaviours associated with dermatillomania often result in the discoloration of skin and eventual scarring. Severe tissue damage can even occur in the most serious of cases. This habit is therefore thought to be a form of self-soothing to assuage feelings of extreme anxiety and depression. The question then is, what causes a person to cause pain and unwanted damage to themselves?
What Triggers Onset?
There is a high comorbidity between body-focussed repetitive behaviours (BFRBs) like dermatillomania and other mood disorders, but a direct causal relationship has not been found. However there is a question as to whether the reaction to the symptoms of mood disorders could trigger the onset of BFRBs such as dermatillomania. For many people with mental disorders a history of trauma is often found. The word “trauma” is used to describe experiences or situations that are emotionally painful and distressing, and that overwhelm people’s ability to cope mentally. Trauma has been shown to lead to destructive habits such as addiction as the person seeks ways to escape the overwhelming feelings of anxiety and tension which builds up as a result of the trauma.
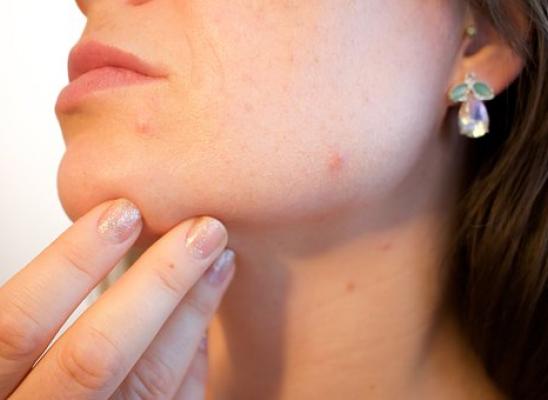
Dermatillomania is triggered by many reasons. For many patients, skin picking first begins with the onset of acne as a teenager. The acne is usually scratched at and picked at. The compulsion to scratch and pick the skin continues even after the acne has vanished. Other types of skin conditions can act as the onset for dermatillomania. These commonly include keratosis pilaris, psoriasis, and eczema. It is important to note that grooming the skin with these conditions can be normal. However, those with dermatillomania exhibit excessive grooming disproportionate with the severity of the skin condition.
Whether skin picking is brought about by acne or another skin condition, the majority of cases first arise in teenage stage. Dermatillomania also commonly first occurs in adults, usually the common age of onset is 30 years old to 45 years old. Onset at this age can occur for the same reasons: acne and other skin conditions. It is also related to stressful life events. These include marital conflicts, death of friends or family, and unwanted pregnancies. Because skin picking is related to Obsessive Compulsive Disorder (OCD), its onset can often be linked up to the onset of other symptoms of OCD. One recent study of those with dermatillomania showed that over 47.5% of those interviewed started to exhibit skin picking behaviours before the age of 10.
Response to trauma
Although the cause of this compulsive disorder is largely unknown, it appears that trichotillomania can be triggered by an initial trauma, thus indicating that this particular disorder is ‘response’ behaviour, rather than a stand-alone illness. Trauma in childhood such as physical or sexual abuse, loss of a loved one, or any emotional problem such as divorce could cause a young child or even an older one to begin picking their skin. During periods of tension, anxiety, or stress, patients exhibit the uncontrollable urge to pick, squeeze, or scratch the skin. Many individuals suffering from dermatillomania cannot pinpoint the exact moment they started pulling, but a large number of them do remember it starting around the time of some upheaval or traumatic incident in their lives. Once the urge to pick turns into a compulsion it becomes almost impossible for the person afflicted with the condition to stop without some type of intervention or support from a friend or family member.
Pharmacological Treatment
There are several different types of pharmacological treatment for skin picking disorder. The most commonly known type of treatment is Selective Serotonin Reuptake Inhibitors (SSRI). These have been shown to be highly effective in treatments for OCD. Because of this, they have been widely used for treating dermatillomania. Clinical studies have not shown any clear support of this because tests involving double-blind placebos have not yet been completed. Doxepin, clomipramine, naltrexone, andolanzapine, and pimozide have also been effective and helpful in the reduction of skin picking behaviours.
Behavioural Treatments
Behavioural treatments for dermatillomania are more common than pharmacological treatments. These treatments include cognitive-behavioural therapy (CBT), acceptance and commitment based therapy (ACT), dialectical behavior therapy (DBT), and habit reversal training (HRT). Habit reversal, in particular, has been shown to be effective., encouraging patients to keep themselves busy by occupy their hands throughout the day, with fidget toys for instance, has also shown success at treating the disorder. Dermatillomania, or skin picking disorder, is surprisingly a prevalent problem worldwide.
The vicious cycle
Dermatillomania affects a surprising large number of people worldwide. Though the research is not set in stone, the most recent findings suggest that it affects between 2% to 3% of the general population. Furthermore, many cases are gone unreported, are not recognized, or are not given any public/media attention. This means that the actual prevalence of dermatillomania could be significantly higher. The person suffering from dermatillomania may want to stop but she is continuously bombarded with messages of perfection which she feels is impossible to attain. Another problem which results in further trauma is the sense of isolation sufferers feel. Most, if not all family members are unable to understand the condition and are often quick to judge the person, which is why most people afflicted with the disorder don’t report it.
Online test
Find out the severity of your symptoms with this free online test
Start your journey with SkinPick
Take control of your life and find freedom from skin picking through professional therapy and evidence-based behavioral techniques.
Start Now